The Future of Birth Control: We Talk to Megan Tantillo
Imagine a world where a variety of birth control methods were free and accessible. All people made an informed decision regarding which contraception best suited his or her unique needs.
Unfortunately, that is not our reality.
Take a look at these results from a poll I took on Instagram:
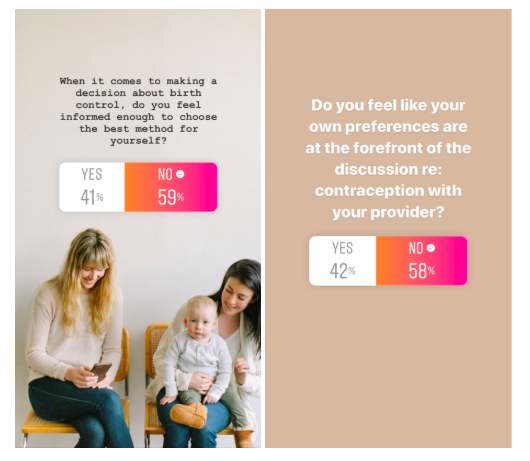
59% of women believed they didn’t feel informed enough to choose the best method of birth control for themselves.
58% of women felt like their preferences were not at the forefront of the contraception discussion with their providers.
And this is not just a problem on Instagram. The truth is, there are global knowledge gaps in reproductive health, especially when considering contraception.
When it comes to selecting contraception, you and your provider share responsibility in the decision making process. This is the responsibility to have a frank conversation about your reproductive health goals, preferences, lifestyle and also your health risks.
Of course the approach is highly individualized — meaning the birth control your friend chooses may not be the right fit for you. Which is why it is important for you to arrive at your appointment with some background knowledge, so you can have a meaningful discussion with your provider about which method will work for you.
In an effort to fill those knowledge gaps about birth control, for World Contraception Day, I am partnering with Natural Cycles to start a conversation. An open and honest conversation about birth control, which will hopefully give you some insight regarding your options, and empower you to make an informed choice for yourself!
Founded in 2007, World Contraception Day takes place on the 26th of September every year. The global campaign raises awareness of birth control and pushes for better education when it comes to sexual and reproductive health.
What stories frequently surface when you speak to patients about birth control? What is on their mind? Do they feel informed enough to choose the best method for themselves?
For complete transparency, most conversations I have with my clients about birth control are based on the following questions:
How do I prevent pregnancy without hormonal contraception?
and
How do I transition off the Pill?
To be clear, for many women, the Pill is a sensible choice. However, given the nature of my work, teaching women how to balance hormones naturally, this usually involves discussing side effects of the Pill, and hormone-free contraception options that perhaps were never considered before.
When speaking to clients about birth control, many women are surprised by the Pill’s mechanism of action. They are unaware of how the Pill works, and side effects are seldom discussed. For instance, many combined oral contraceptives are linked with depression, leaky gut, nutrient deficiencies such as magnesium, B12 and folate, as well as fatigue and thyroid dysfunction, among other symptoms.
I’m not against the Pill. However, it needs to be prescribed and taken responsibly. There are health risks involved and it’s important for you to know both sides of the story before you make a decision.
Another story that frequently surfaces when speaking with clients about birth control is they were told the Pill or an other hormonal method of contraception would balance hormones.
This couldn’t be farther from the truth. The Pill is a reliable contraceptive — greater than 99% effective with perfect use, however, it does not balance hormones. Spoiler alert: The Pill won’t fix your period. It simply supplies a dose of hormones preventing ovulation and therefore a pregnancy from occurring. The pill is a trusted contraceptive – however, if you are looking to balance hormones naturally, it is not the right choice for you. Non-hormonal methods such as Natural Cycles for instance, don’t suppress ovulation. By measuring your basal body temperature, you get to know your unique cycle, and prevent or plan for a pregnancy, all while avoiding unwanted side effects. That’s a win-win!
What changes/innovation is needed to ensure that women’s own preferences will be at the forefront of the discussion of contraception?
In order to ensure women’s preferences are kept at the forefront of contraception discussions, they must be educated. Healthcare professionals like myself must consider this a call to action.
Now more than ever, we need to empower women to be their own health advocates and act as equal partners in their healthcare. We must continue to spread awareness and knowledge because our reproductive health depends on it. Knowledge truly is power.
It’s important to understand that although patient preferences are a top priority, there are other important factors that need to be considered, too. For instance, certain medical conditions may exclude options. Have a history of blood clots? The Pill is not for you. Multiple partners? Consider condoms.
In order to meet the changing needs of our patients, we must be online. A huge part of the problem for many women is access. In addition to this, counseling, insurance issues, language barriers, cultural differences, protocol for consent and a time out is challenging to complete in a single appointment.
Telehealth services have promising potential to expand access to expert care. Services to include on demand nursing staff to answer questions regarding options, preferences, health risks, etc. would ensure women have trusted and accurate information, allowing her to consider which method would work best for her, and ultimately provide true informed consent.
To enable informed choice of birth control, it can be important for women to consider how their overall health is impacted by their menstrual cycle. This can nonetheless be difficult to understand without tracking it carefully as all cycles are unique. What difference do you think technology can make in this aspect?
In the eCourse I teach, The Period Fix, I often refer to the menstrual cycle as a female vital sign — or a gauge of overall health. Menstruation should be easy and pain free, and without tracking, it is difficult to pinpoint problem areas.
There is much to consider when beginning to understand and track your menstrual cycle. Changes to cervical mucus, basal body temperature, cravings, energy, libido, mood, sleep, digestion even changes to our skin and hair — all of these factors should be considered when tracking cycles.
Imagine tracking all of these variables and charting your data by hand on your own? How overwhelming does that sound? Technology simplifies this process and makes cycle tracking possible for many women. Now more than ever women have access to their cycle data with the ease of an app.
When asked, “When was your last menstrual cycle?” Almost all of my clients reach for their phone.
What is the experience of your patients with tracking symptoms and moods in relation to their cycles? How does tracking impact your patients’ lives?
It is life-changing!
Many women for the first time understand how their bodies work and can make sense of how they feel on a day to day basis. With knowledge of cycle changes and hormone fluctuations, women are able to support their health in much more meaningful ways throughout the month.
For instance, my clients understand that after ovulation, energy typically dips and they are more prone to stress. I coach them to set boundaries, minimize plans, and focus on self-care. They understand cooked foods are easier to digest and supplementing with magnesium can help avoid cramps and unwanted stress at this time.
Tracking enables women to understand their cycles, better care for themselves to promote natural hormone balance and feel good in their bodies.
What do you see as the connection between enabling women to freely choose their preferred method of birth control and women’s empowerment in general?
The connection between women freely choosing her preferred method of birth control and women empowerment is knowledge. Knowledge truly is power. When you can take charge of our health with confidence, that is power.
The ultimate decision on how to care for your health is your own. As a nurse, all patient outcomes we know are dependent on the individuals understanding of that. My ultimate goal is to always share both sides of the story in reproductive health and beyond, and believe it or not, in the end, most of my clients choose a non-hormonal means of contraception on their own.
Megan Tantillo BSN, RN is the founder of Holistic Health Code, on a mission to provide accessible holistic care and education for all. Megan is currently pursuing her Doctorate in Nursing Practice with special interest in women’s health and telehealth technologies.
Did you enjoy reading this article?
