Menstrual cycle: Overview & how you feel in different phases
Follows NC° Editorial Policy
At Natural Cycles, our mission is to empower you with the knowledge you need to take charge of your health. At Cycle Matters, we create fact-checked, expert-written content that tackles these topics in a compassionate and accessible way. Read more...
Key takeaways
-
The menstrual cycle is a series of events, set in motion by fluctuating hormones, that prepares the body for pregnancy
-
There are multiple phases of the menstrual cycle, the most well-known of which is the period
-
By tracking your menstrual cycle and ovulation, you can learn what is normal for you and better spot any abnormalities, such as an unusually long or short cycle or period bleeding that is heavier or lighter than usual
On this page
- What is the menstrual cycle?
- How long is a typical menstrual cycle?
- What are the different phases of the menstrual cycle?
- How do you feel at different stages of the menstrual cycle?
- Temperature & the menstrual cycle
- At what age do girls usually get their period?
- How does your period change over time?
- What is an irregular period?
- What causes cycle irregularities?
- Tracking your period
- When to see a doctor
- More than a period tracker
The menstrual cycle plays a crucial role in our health, and there is so much to know about this fascinating process that follows us throughout our lives. Whether you consider yourself well-informed or are just starting on a journey to understand your menstrual health better, knowing your cycle is a great way to get to know your body. Here’s everything you need to know about the menstrual cycle, its different phases, the hormones involved, how to spot irregularities, and how tracking your cycle can help you plan or prevent pregnancy.
What is the menstrual cycle?
Your menstrual cycle is a series of events your body goes through in preparation for and facilitation of pregnancy. Each cycle has two distinct phases, starting on the first day of your period and controlled by fluctuating hormones. The menstrual cycle ends the day before your next period, and the next cycle begins when your period starts [1].
How long is a typical menstrual cycle?
The length of the menstrual cycle varies among individuals, with normal cycles usually ranging from 21 to 35 days [23]. While the average length is often considered 28 days, Natural Cycles research examined over 600,000 cycles and found that only 13% of cycles in the study group were 28-days long, with 29.3 days as the average [3].
It’s also worth keeping in mind that some menstrual cycles are very regular, while others are more variable. We will explain more about irregular cycles and potential causes later in this article.
When does ovulation usually happen?
Traditionally, the medical world has advised that ovulation usually occurs around day 14 of your cycle, near the midpoint (and 14 days before your next period). However, recent research finds that ovulation timing varies drastically. One study found that, out of 69 cycles lasting 28 days, only 10% ovulated on day 14. Instead, ovulation occurs between days 10 and 22 [4]. There are also cases when ovulation is even less predictable, particularly if you experience irregular cycles, have just started your periods, or are entering perimenopause.
What are the different phases of the menstrual cycle?
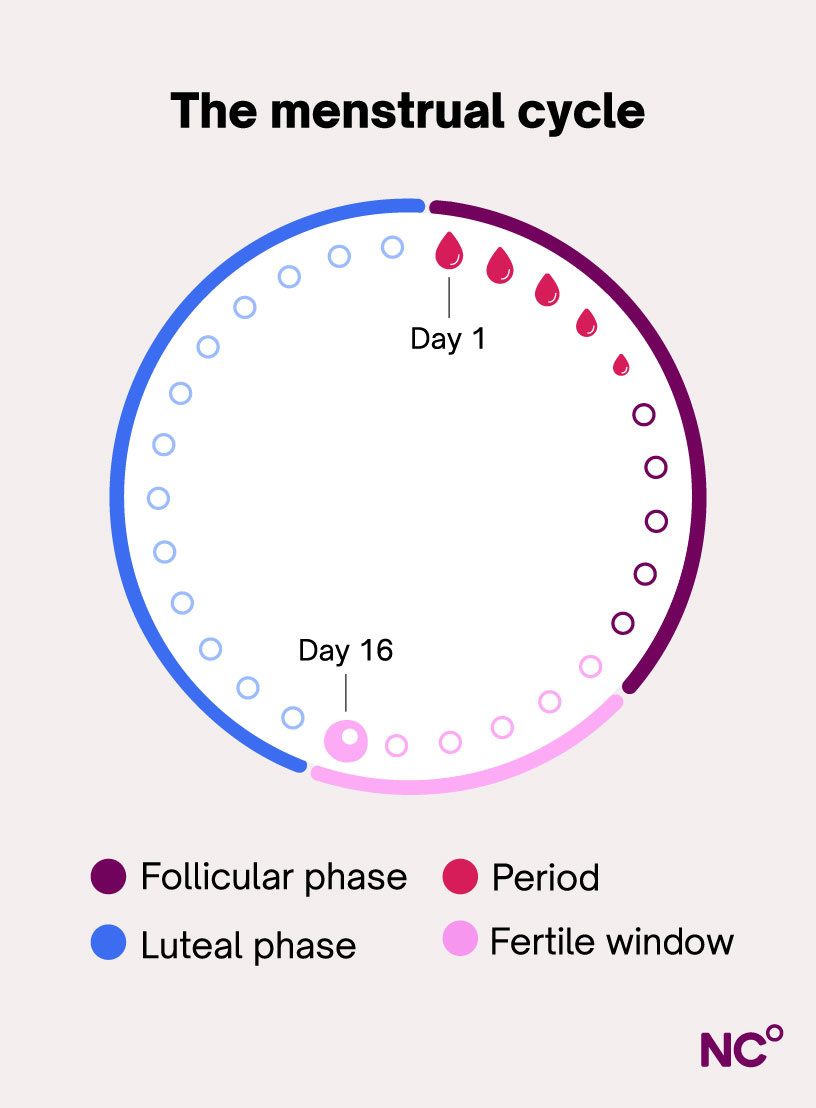
There are two phases in the menstrual cycle: the follicular and luteal phases. Within these, you also have two significant events: your period and ovulation. Each phase and event of the menstrual cycle plays a unique role. But the cyclical nature of each is essential to the others, and together they are pivotal to the cycle as a whole. It’s a fine balance of hormones and biological triggers that keeps the cycle going.
Period
Every cycle begins with menstruation, more commonly known as your period. Your period is the cycle phase we are most aware of because of its physical manifestation as a bleed. It begins on the first day you notice bleeding and ends on the day bleeding stops, usually lasting two to seven days [2]. Typically, you lose around one to five tablespoons (20 to 90ml) of blood each period, but some women may have heavier periods. This bleed is your uterus shedding its lining and releasing it through the vagina [5]. We will explain the creation and purpose of the uterus lining in more detail in the following phases.
Follicular phase
The follicular phase begins on the first day of your period (overlapping with the menstruation phase) and ends with ovulation. This phase is the most variable in length across individuals, and some research suggests it lasts, on average, 10 to 16 days [6]. However, a Natural Cycles study estimated that the follicular phase lasted an average of 16.9 days and decreased by approximately 0.19 days per year between the ages of 25 and 45 [3].
The follicular phase is responsible for the maturation of undeveloped egg cells, known as ovarian follicles (hence the name “follicular”), that prepare the eggs for potential fertilization [6]. This process is triggered by hormones, most notably follicle-stimulating hormone (FSH) and estrogen. FSH supports the development of several egg cells until a single dominant egg cell prevails [7]. This dominant egg cell produces estrogen, which suppresses FSH and stops the maturation of other follicles [8]. Estrogen also plays a second role in the follicular phase, thickening the uterine lining, which later plays a critical role in implantation if an egg is fertilized [7]. Estrogen levels reach their peak one or two days before ovulation, followed by a surge in luteinizing hormone (LH) and FSH, which trigger the release of the mature egg cell [7, 8]. Fun fact: Women are already born with all of their egg cells [9]!
Ovulation
Ovulation is the release of a mature female egg cell from an ovary, which takes place at the end of the follicular phase [6]. It occurs around one to two days after the surge in LH hormone, which is why many at-home ovulation tests are designed to detect high LH levels in urine, indicating that ovulation may be about to occur [10].
Once released, the egg cell survives for 12-24 hours, during which it can be fertilized by a sperm cell [11]. After this time, the egg cell dies, and your fertile window — the time during which sex can lead to pregnancy — ends. This window is typically six days long, including the 24 hours after ovulation, and five days prior, since sperm can survive for up to five days in the female reproductive system [3].
Luteal phase
The final phase of the menstrual cycle is the luteal phase, which takes place after ovulation and before your next period. The length of the luteal phase is relatively consistent across individuals, typically lasting about 14 days [6]. Right after ovulation, estrogen levels drop, and the corpus luteum (a temporary gland formed from the follicle after ovulation) produces progesterone. This hormone continues the preparation of the uterus lining for implantation of a fertilized egg [6]. If the egg is not fertilized, progesterone levels fall, and the uterus lining sheds, resulting in your period [6]. And so the cycle begins again!
How do you feel at different stages of the menstrual cycle?
You may be unaware of your changing hormones, but our bodies often give us hints that these changes are happening. It is common for our energy levels, physical symptoms, and moods to change as our hormones do.
- Period: Your bleed is the main symptom of your period. Sometimes the sensation of bleeding from your vagina can feel uncomfortable, especially if you have just started your periods and aren’t used to it yet. Keeping pads, tampons, or period pants on hand can help you feel prepared and ease discomfort if your period starts unexpectedly. During the first few days of your period, you may also feel continued symptoms of premenstrual syndrome (PMS) that often start in the luteal phase. PMS is different for everyone, but common physical symptoms include cramps, digestive issues, and sore breasts [12].
- Follicular phase: After your period ends, both estrogen and progesterone levels are low [14]. As estrogen increases in the latter half of the follicular phase, many women feel more energetic, more social, and less anxious [13].
- Ovulation: Some women report experiencing ovulation pain, also called Mittelschmerz. This is usually mild pain on one side of the body, where the ovary is releasing an egg, and can feel like a stabbing pain or a dull ache [15]. You might also have a higher sex drive and more energy, as your hormones spike and you reach your peak fertility [16].
- Luteal phase: It is during the luteal phase that PMS symptoms can begin, indicating your period might be coming. Whilst the physical symptoms mentioned above are often the most widely acknowledged, it is not uncommon to also experience mental and emotional symptoms, including irritability, anxiety, mood swings, problems with concentration or memory, and feelings of sadness [12].
It’s important to remember that everyone’s experience of hormonal changes will be unique. You may not notice any symptoms at all, or you may notice more severe symptoms. Very severe PMS is known as premenstrual dysphoric disorder (PMDD) [12]. If you have any concerns about symptoms or think you may have PMDD, speak to your healthcare provider.
Temperature & the menstrual cycle
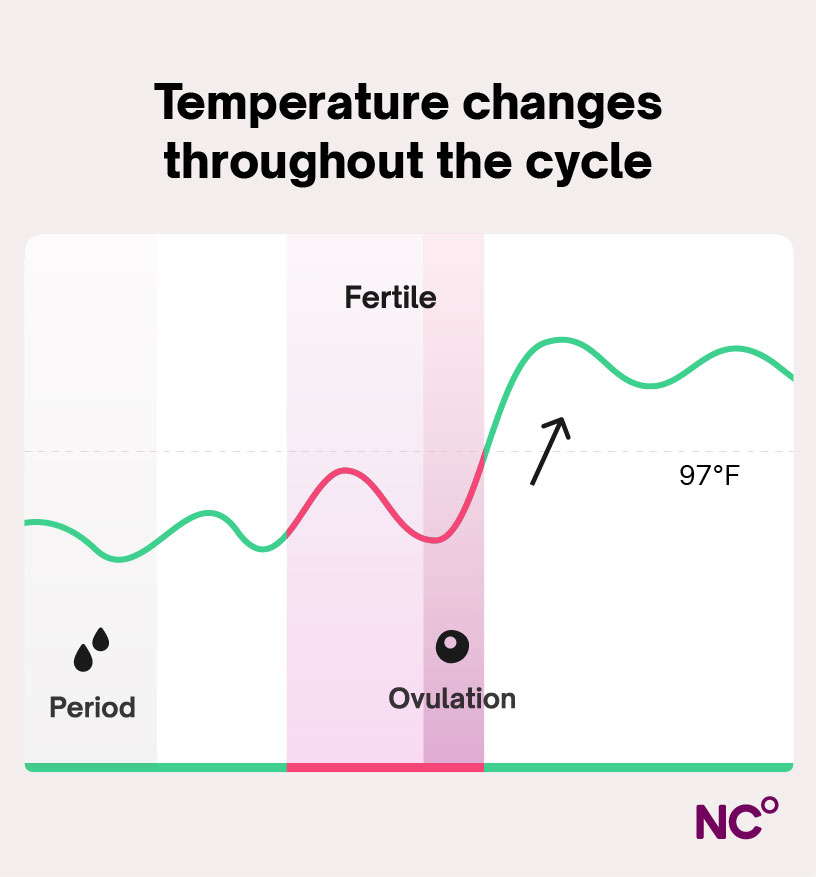
Another fascinating change in your body throughout your menstrual cycle is fluctuations in basal body temperature (BBT). BBT is your body’s lowest resting temperature, typically measured when you first wake up, before any activity or during sleep by a wearable device [17, 18]. In normal ovulatory cycles, your BBT follows a clear pattern. It is lower during your period and follicular phase. Then, after ovulation, it increases by a small but notable amount and stays high until around the time of your next period [17].
Since 24 hours after ovulation marks the end of the fertile window, we can use BBT as a fertility awareness method to plan or avoid pregnancy. Natural Cycles is the first FDA-cleared birth control app that uses biomarkers, such as body temperature, and a first-of-its-kind algorithm to predict the fertile window so you know when it is safe to have sex while avoiding pregnancy.
At what age do girls usually get their period?
Periods typically start around age 12. But they can start from as early as age 8, and most will have regular periods by age 16 to 18, but it can take a few years for cycles to become more regular [2, 19]. Other signs of puberty, such as growing underarm and pubic hair, can indicate your body is going through puberty and getting ready to start having periods. Your first period usually arrives around two years after your breasts have started to develop [2]. It is normal for your first few periods to be light, last only a few days, and involve only some spotting of reddish-brown blood, but this, too, can vary from person to person [20].
How does your period change over time?
It is normal for our periods to change as we age. When you first start your periods, they can be irregular. Typically, periods become more regular by age 18 and maintain the same characteristics (cycle length, heaviness of flow, and duration of flow) throughout our fertile years [2]. The exception to this is pregnancy, when periods typically stop altogether until after birth. Some individuals may experience bleeding during pregnancy, but this is not technically a period.
Fertility starts to decline after the age of 30, and at a greater pace after mid-thirties [21]. As you enter your 40s, you may notice your cycles are getting significantly shorter or your periods are either lighter or heavier, which can be an indication that perimenopause is beginning [1]. Perimenopause is the transition our bodies go through in the final years of our fertility, before reaching menopause. During perimenopause, our menstrual cycles get shorter, ovulation occurs earlier, and periods become more irregular [3, 22]. Menopause is the time of our final period, determined retrospectively after 12 months without a period [23].
What is an irregular period?
Irregular periods can be determined by their frequency, the amount of bleeding, and the length of your period. Some characteristics that might be considered irregular include [24]:
- Periods that are less than 21 days or more than 35 days apart
- Periods that are suddenly changing in length, even if within the range above
- Not having a period for more than 90 days
- A very heavy or very light flow – compared to what’s normal for you
- A period that lasts longer than 7 days
- A period that soaks through one or more tampons or pads each hour
- Bleeding after menopause, between periods, or after sex
It’s very common to have some irregularities in your cycle, and up to a quarter of us will experience irregular cycles at some point in our reproductive years [25]. But if you notice lots of changes or are concerned about any symptoms, you should always speak to a healthcare professional for advice and evaluation.
What causes cycle irregularities?
Many factors, including natural hormonal changes, lifestyle influences, and gynecological conditions, can cause cycle irregularities. Let’s look at some of the most common causes of irregular periods and menstrual cycles.
- Pregnancy: If your period is late or missed, and you have recently had unprotected sex, there is a chance you might be pregnant. To check, you can take an at-home pregnancy test from the first day of your missed period or speak to a healthcare practitioner.
- Puberty: It is normal for your periods to be irregular when they first start, and it can take up to six years for them to settle into a regular pattern [20].
- Perimenopause: As we approach the end of our fertile years, it is normal for periods to become more irregular as hormone levels fluctuate erratically, and we may experience anovulatory cycles [22].
- Stress: Did you know that stress might affect your menstrual cycle? Stress can disrupt hormone production, which in turn can make your period late or stop it from coming altogether, by preventing or delaying ovulation [26].
- Low or high BMI: Weight impacts many aspects of our health, including the menstrual cycle. Studies have found that being either severely underweight or overweight can sometimes lead to anovulation and infertility. The good news is that weight management may restore a regular menstrual cycle and fertility [27, 28].
- Thyroid conditions: Problems with your thyroid may cause irregular cycles, as it helps regulate hormones, including estrogen and progesterone. An underactive thyroid (hypothyroidism) can be linked to heavier and more irregular periods, while an overactive thyroid (hyperthyroidism) may cause lighter, less frequent, or missed periods [29].
- Polycystic ovary syndrome (PCOS): PCOS is a condition in which you have high levels of androgens (a type of hormone), which cause the disruption or absence of ovulation. While many individuals with PCOS show no symptoms at all, it is one of the leading conditions causing irregular periods [30].
- Endometriosis: If you have particularly painful and heavy periods, there is a chance you may have endometriosis. This condition is characterized by the growth of uterine tissue outside of the uterus, usually on the ovaries, fallopian tubes, or other pelvic structures [24].
If you have any concerns about irregular periods, think you may have PCOS or endometriosis, or are worried about lifestyle influences on your cycle, speak to your doctor or healthcare provider.
Tracking your period
One way to know whether your period and menstrual cycle are normal is to track them. Doctors often ask what day of your cycle you are on, for example, when you get your pap smear, and knowing this information can help healthcare providers get a better view of your reproductive health.
You can use a diary or online calendar to mark the first day your period starts, and the last day you experience bleeding. This will help you visualize how long your periods last and how long your cycle is. You can also make additional notes to yourself about how heavy your bleeding is, any PMS symptoms you are experiencing, and anything unexpected, such as spotting. However, tracking period dates alone doesn’t tell the whole story.
Natural Cycles shows you a more detailed picture of your reproductive health. Using biomarkers and our first-of-its-kind algorithm, the NC° app will do the hard work for you to predict ovulation and the fertile window, and provide a personalized report on overall cycle length, phases, and period length, as well as any symptoms you have recorded.
When to see a doctor
Always speak to your doctor or healthcare provider if you have any concerns about your menstrual cycle, especially if:
- You notice your cycle is often longer than 35 days or shorter than 21 days
- Your period flow has changed and is much lighter or heavier than usual
- Your period lasts for longer than 7 days
- You haven’t had a period for more than 90 days
- You notice spotting between periods
- You experience pain or bleeding during sex
- You think you may have a gynecological condition, such as PCOS or endometriosis
- You think you have a sexually transmitted infection
More than a period tracker
At Natural Cycles, we’re dedicated to providing a birth control option that’s not only hormone-free but can also help you learn more about your unique menstrual cycle and wider reproductive health. As well as an FDA-cleared form of contraception, you can use the NC° app to track PMS symptoms, predict your period, and plan pregnancy. Natural Cycles is here to guide you through all stages of your fertility journey. Find out how it can support you today!
Did you enjoy reading this article?
